You are what you eat, but does it show up in your blood?
What's covered?



You can see what’s on your plate, but you can’t see what’s in your blood. We analysed anonymised blood test data from Thriva users to find out how what you eat really shows up in your blood and whether supplements are closing the gaps.
The way we choose to eat is personal, and different diets come with different nutritional trade-offs. This isn’t about proving one diet is better than another; it’s about helping you understand the broad trends so you can make informed choices about your nutrition and how you monitor your health.
Our methodology: How we selected and analysed diet type data
We analysed blood test results from Thriva users, collected over a two-year period, who follow one of six dietary patterns—omnivore, vegetarian, vegan, pescatarian, flexitarian, and paleo—to see how the food choices people make actually show up in biomarkers directly related to nutrition.
We also looked at supplementation patterns for vitamin D, B12, and iron to see whether people are filling the gaps in their diets.
Our users are a self-selected, UK-based, health-conscious cohort, so these results likely reflect people already paying more attention to their nutrition than the general population. We have less data for smaller groups (like paleo), which may influence how reliable our findings are.
This article looks at observational trends, which means that differences between groups could be influenced by age, sex, body composition, supplement use, and other factors we haven't adjusted for.
We've used median values throughout because most of these biomarkers aren't normally distributed, and medians give a more accurate picture of what's typical, which is less affected by outliers.
Folate: The nutrient that plant-based diets deliver best
Folate is a B vitamin involved in DNA synthesis, red blood cell production, and cell division. It's found in leafy greens, legumes, fortified grains, and some fruits.
While folate is important for everyone, it's particularly important during pregnancy, as low folate is a well-established risk factor for neural tube defects. Outside of pregnancy, low folate can contribute to a type of anaemia called megaloblastic anaemia. It’s also associated with raised homocysteine, a marker linked to cardiovascular risk.
Because plant-based diets tend to be richer in folate-containing foods, you'd expect higher folate levels in those groups—and that's exactly what the data shows.
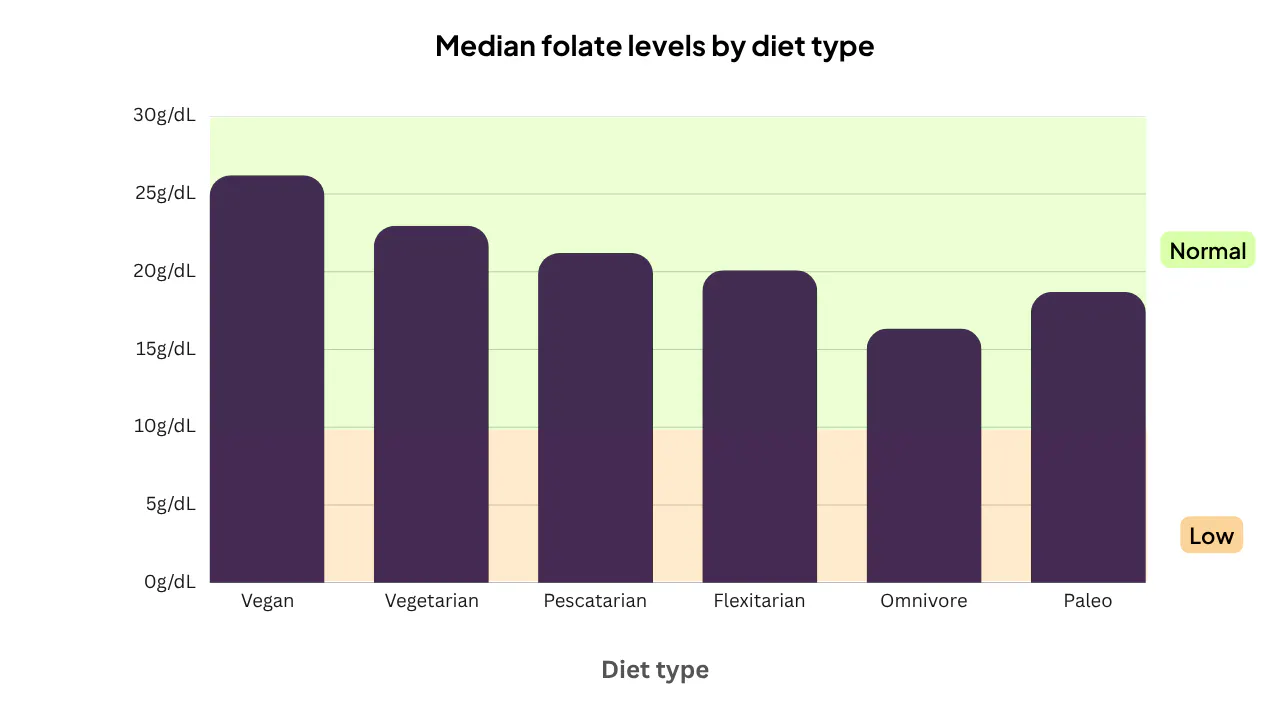
This is consistent with published research on large groups of people. The EPIC-Oxford study, a large UK-based cohort study, found the same pattern in British men.
There's a clear dose-response pattern in our data, which means that the more plant-focused the diet, the higher the folate levels.
Key takeaway
Folate is one nutrient where eating more plants consistently shows up in blood results. If your diet is low in leafy greens and legumes, it's worth checking.
Ferritin: Where meat-based diets have the advantage
Ferritin is a protein that reflects your body's iron stores. When ferritin is low, it means your iron reserves are running down, which can happen well before you develop anaemia.
Low iron stores are associated with fatigue, reduced concentration, and impaired exercise capacity.
Iron in food comes in two forms: haem iron (found in meat) and non-haem iron (found in plant foods). Haem iron is absorbed roughly two to three times more efficiently than non-haem iron, which is why iron status may be a concern for plant-based eaters.
Our data reflect this, as paleo users had the highest median ferritin, followed by omnivores.
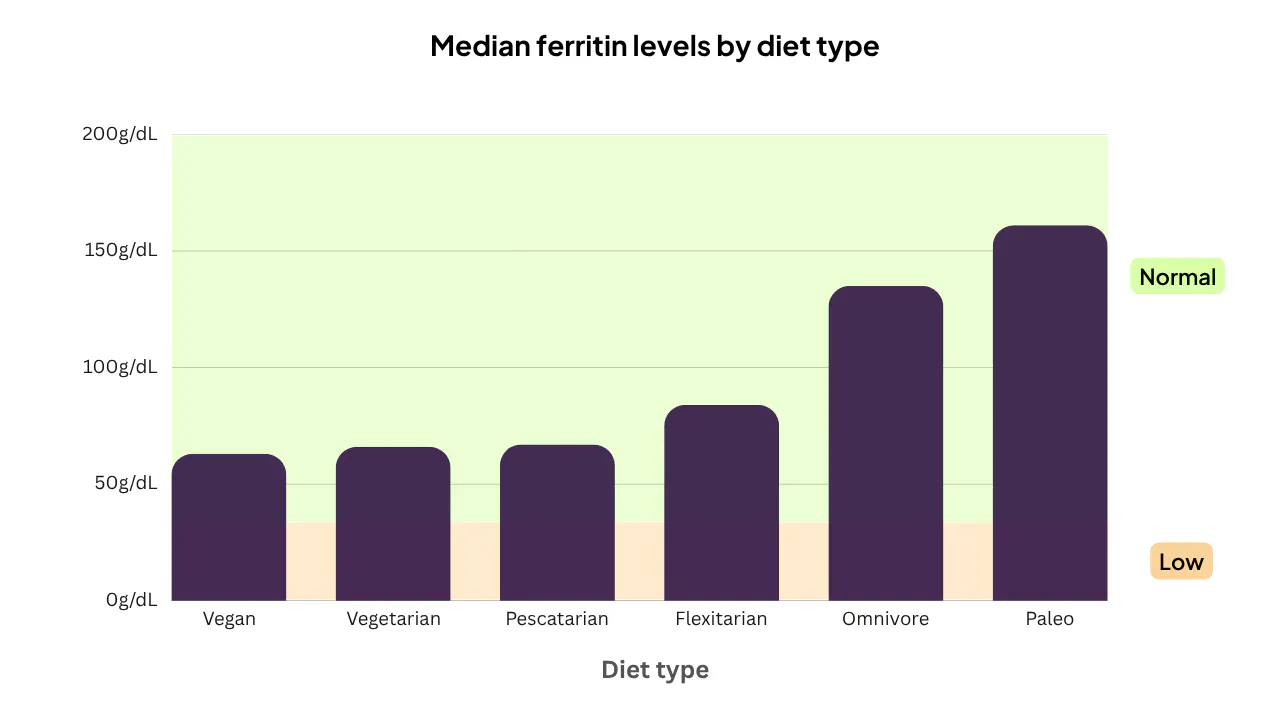
Our findings are consistent with published evidence: for example, a 2018 systematic review and meta-analysis found that vegetarians had ferritin levels roughly 30 µg/L lower than non-vegetarian controls.
Ferritin can also be elevated by inflammation, though, which is why an iron panel gives you a more complete picture than ferritin alone.
Are people supplementing iron?
Iron was the least commonly supplemented nutrient in our data, with just 5% of users reporting taking an iron supplement.
However, iron is one supplement where more isn’t better, and too much can be harmful.
You should always discuss low ferritin levels with your doctor before supplementing, so that a cause for your low ferritin can be determined. This is because low ferritin can cause anaemia, which can be a sign of underlying medical issues.
Key takeaway
Plant-based diets are consistently associated with lower ferritin in both our data and published research. If you follow a plant-based diet, especially if you menstruate or exercise heavily, it’s a good idea to track your iron status.
Vitamin B12: The supplement that’s important for plant-based eaters
Vitamin B12 is crucial for nerve function, DNA synthesis, and red blood cell production. It's found almost exclusively in animal products, which is why it’s often a concern for vegetarians and vegans.
However, most of the vegan users in our sample had adequate B12 levels. Since B12 is practically absent in vegan diets (with the exception of fortified foods), this indicates that some vegans are taking supplements.
A 2023 cross-sectional study of German omnivores, vegetarians, and vegans found that supplemented vegans had B12 status comparable to omnivores, which supports this finding.
Around 30% of vegan users in our data fell into the "deficient" or "possible deficiency" category, which is the highest proportion of any dietary group.
So while the typical vegan user appears to be supplementing effectively, some are still falling short.
Who is supplementing B12?
About 24% of Thriva users reported taking a B12 supplement. The data shows a mix of B12 results within both supplementers and non-supplementers.
It’s a reminder that supplementation isn't a guarantee: dose, form, consistency, and individual absorption all affect whether a supplement actually shows up in your blood test results.
Key takeaway
Supplementation clearly helps, but 30% of vegan users still had suboptimal levels. If you follow a plant-based diet, a blood test can tell you whether or not a supplement could help.
Vitamin D: The most-taken supplement among Thriva users
Vitamin D supports bone health, immune function, and mood. Unlike the other nutrients in this article, vitamin D status is primarily driven by sunlight rather than food, which is why the NHS recommends that nearly everyone in the UK consider supplementing during autumn and winter.
Nearly half (44%) of Thriva users reported taking a vitamin D supplement, making it the most commonly supplemented nutrient by a wide margin, ahead of B12 (24%) and iron (5%).
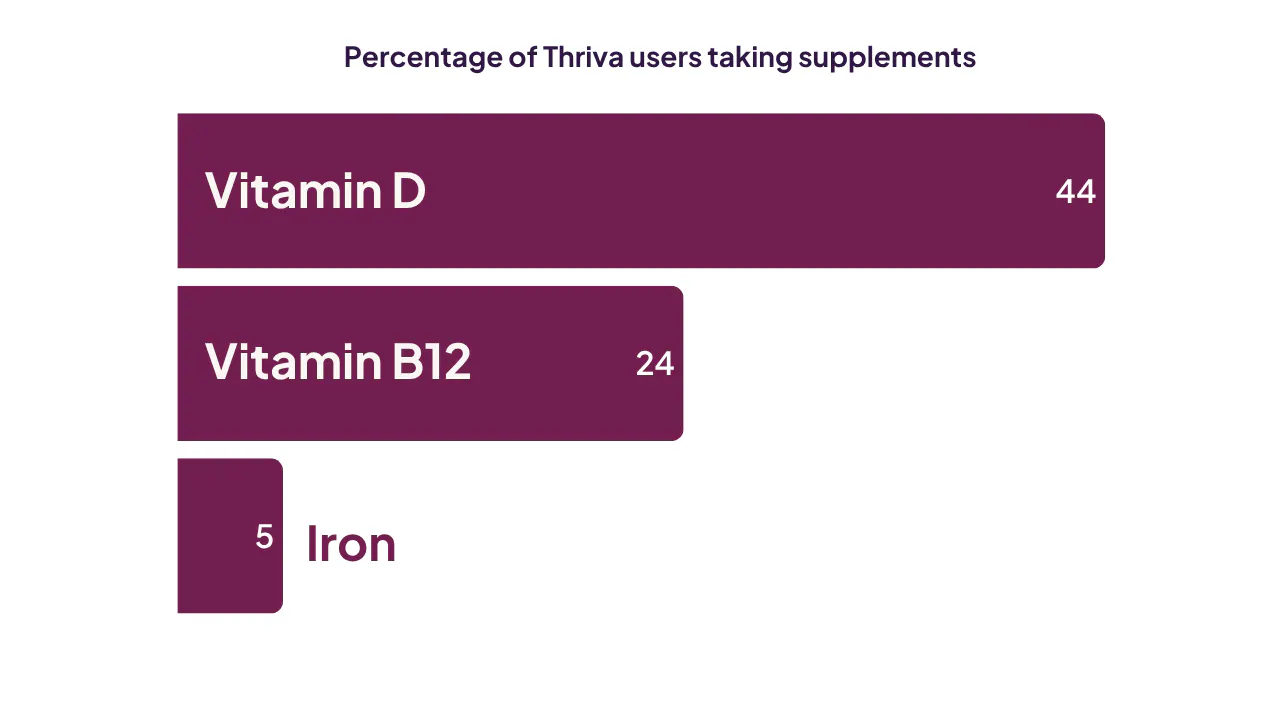
Our data also suggest that supplementation is associated with better vitamin D status. Among users who didn’t supplement, a higher proportion showed deficient or insufficient results (24%) compared to those who did supplement (8%).
The 44% supplementation rate is higher than national estimates of around 26–30%, which likely reflects this cohort's health-conscious profile.
Key takeaway
Vitamin D is the most widely supplemented nutrient among Thriva users, and the data suggest it's associated with better status. If you're not already supplementing during autumn and winter, it’s a simple step worth building into your routine.
What the data means for you
The pattern in this data is consistent: different diets create different nutritional profiles, and those differences show up in blood test results.
Plant-based diets are associated with higher folate but lower ferritin and a higher risk of B12 deficiency. Omnivorous diets maintain stronger iron and B12 status but may fall short on nutrients concentrated in plant foods.
None of this makes one diet better or worse than another. What it does is make the case for knowing your own numbers. Whatever you eat, your diet has a nutritional signature, and testing is the most reliable way to see what yours looks like.
Where you have gaps, targeted changes, whether that’s eating more leafy greens, supplementing B12, or adding vitamin D through autumn and winter, can shift your numbers in a meaningful way.
Disclaimer: This information is for general educational purposes only and isn’t a substitute for professional medical advice, diagnosis, or treatment. Always speak with a qualified healthcare professional first if you have concerns about your health.
- Ami, N. et al. (2016). Folate and Neural Tube Defects: The Role of Supplements and Food Fortification. https://pmc.ncbi.nlm.nih.gov/articles/PMC4933077/
- Baddam, S. et al. (2023). Folic Acid Deficiency. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK535377/
- Gilsing, A.M.J. et al. (2010). Serum Concentrations of Vitamin B12 and Folate in British Male Omnivores, Vegetarians and Vegans: Results from a Cross-Sectional Analysis of the EPIC-Oxford Cohort Study. https://pubmed.ncbi.nlm.nih.gov/20648045/
- Haider, L.M. et al. (2018). The Effect of Vegetarian Diets on Iron Status in Adults: A Systematic Review and Meta-Analysis. https://pubmed.ncbi.nlm.nih.gov/27880062/
- Jáuregui-Lobera, I. (2014). Iron Deficiency and Cognitive Functions. https://pmc.ncbi.nlm.nih.gov/articles/PMC4235202/
- NHS. (2025). Vitamin D. https://www.nhs.uk/conditions/vitamins-and-minerals/vitamin-d/
- O'Connor, C. et al. (2018). Knowledge, Attitudes and Perceptions towards Vitamin D in a UK Adult Population: A Cross-Sectional Study. https://pmc.ncbi.nlm.nih.gov/articles/PMC6267199/
- Storz, M.A. et al. (2023). A Cross-Sectional Study of Nutritional Status in Healthy, Young, Physically-Active German Omnivores, Vegetarians and Vegans Reveals Adequate Vitamin B12 Status in Supplemented Vegans. https://pmc.ncbi.nlm.nih.gov/articles/PMC10586079/


