Heart health biomarkers: What our community data tells us about healthy lipid levels
What's covered?



While cholesterol is a major contributor to heart disease, understanding how to improve it can feel complicated. For Heart Health Month, we looked at cholesterol data from thousands of Thriva users to find out what's actually associated with better lipid results.
We investigated our anonymised dataset to understand what the biggest opportunities are when it comes to heart health—and what they mean for you.
A note on ApoB
You'll see apolipoproteinB (ApoB) referenced in this article. It counts the number of LDL and other atherogenic particles, which cause plaque to accumulate in your arteries. The evidence suggests it predicts cardiovascular risk more accurately than LDL cholesterol alone.
We've written more about why it matters and what your levels mean.
Lipids play by different rules
To understand which biomarkers are most ‘easily’ moved, we looked at how many Thriva users moved different markers from the abnormal to the normal range. And when we ranked these, we saw an interesting pattern emerge: lipid markers like LDL cholesterol and ApoB appear harder to ‘move’ than others.
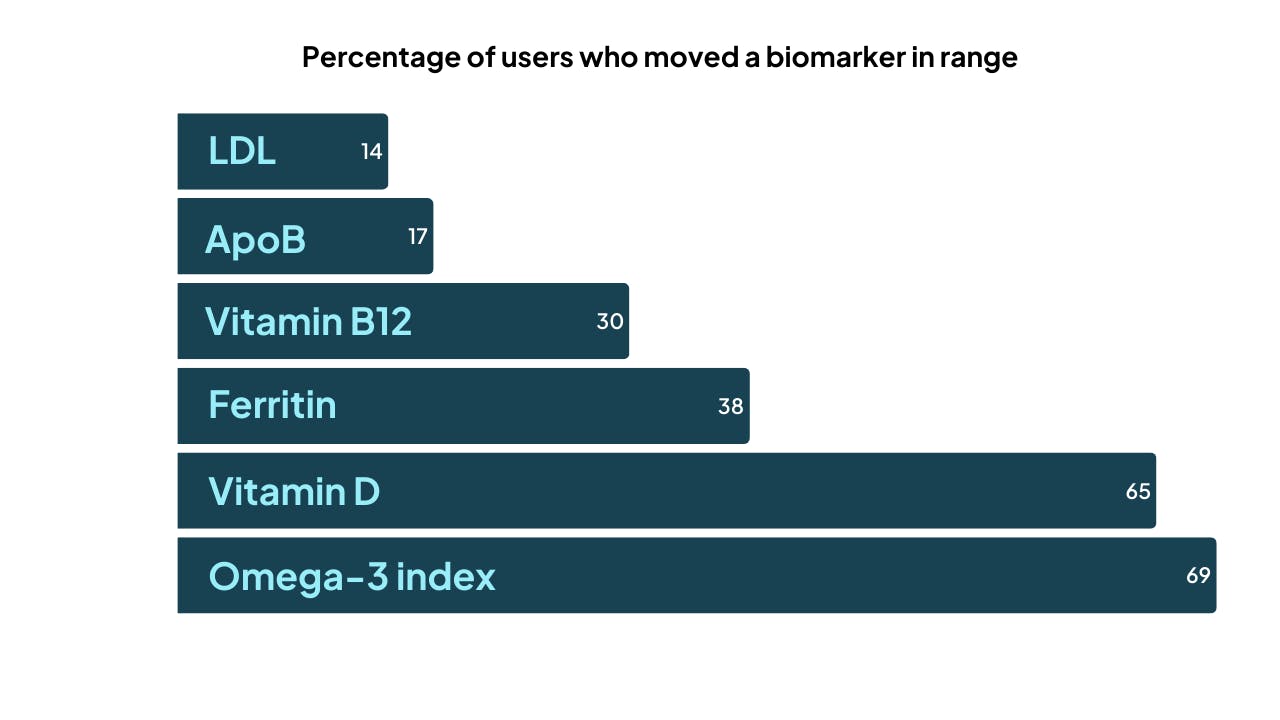
Some of the highest were markers of nutrient adequacy, like vitamin D and ferritin. This makes sense because those markers can be moved by simply adding a daily supplement or making small changes to your diet.
Cholesterol is the output of several systems at once—including diet, movement, alcohol, hormones, and genetics—which means it typically takes a combination of changes, sustained over a longer period of time, to see a shift.
In people with a strong genetic predisposition to unfavourable cholesterol levels, lifestyle changes - whilst incredibly important for overall health and wellbeing - may not always result in meaningful movements.
We don’t see this as discouraging. While it can be challenging to move lipids towards normal and optimal ranges, it’s possible, and we see the Thriva users achieving this through our anonymised data.
To understand which lifestyle factors have an impact, we’ve dug into the data to find out how diet, exercise, and lifestyle changes have helped other Thriva users move their lipid markers.
What you eat matters
Of all the lifestyle factors in our dataset, dietary pattern shows the clearest association with ApoB levels. Plant-based eaters tended to have lower ApoB scores than those who ate meat.
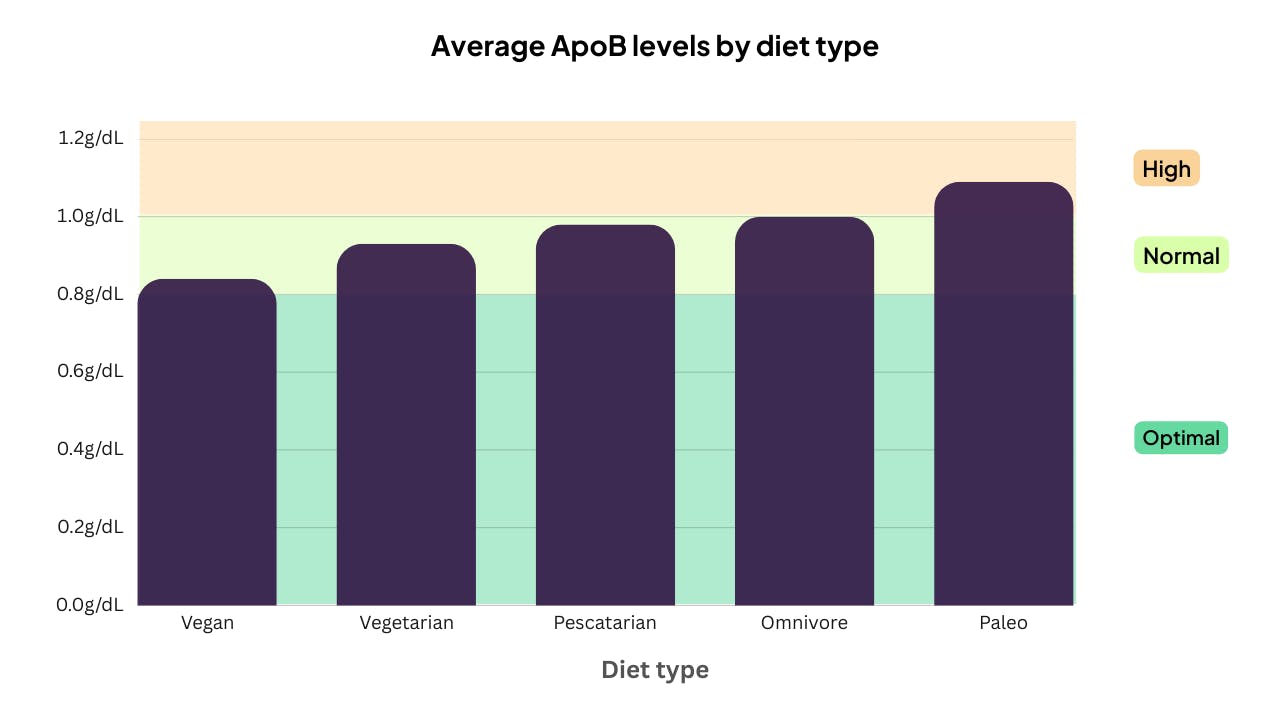
What's likely driving this is the food composition rather than the diet label itself. Diets higher in soluble fibre (from oats, beans, lentils, and fruit) and lower in saturated fat (fat which is solid at room temperature) can reduce the number of atherogenic particles the liver produces. Vegetarian and vegan diets naturally contain more of these foods, which may explain the gradient on our graph.
This is observational, so it doesn't prove diet is the sole cause. Based on research, we know that adding more foods high in fibre, as well as reducing saturated fat, can have beneficial effects on blood cholesterol levels. This means you don’t need to go plant-based overnight—you may just want to make some targeted tweaks to your eating.
However, it’s important to note that females make up a larger proportion of the plant-based eaters in our dataset, which may skew the findings.
Lower alcohol, better lipid results
Alcohol intake shows a clear dose-response pattern in our data, which means the effect scales up with greater intake. Among users drinking fewer than seven units per week, 56.78% have normal or optimal lipid results. This percentage drops in those who consume more alcohol weekly.

This pattern has also been shown in research. According to one large study, consuming more alcohol was linked to worse lipid profiles.
While alcohol doesn’t contain cholesterol, it affects how the liver breaks down fats. Consuming more alcohol can cause your liver to make more triglycerides, which are fats in the blood.
This is one of the more accessible changes in the dataset. It doesn't require a new routine or a dietary overhaul, and even modest reductions appear to be associated with better lipid profiles.
Male and female cholesterol follow different trajectories
One of the most striking patterns in our data is the crossover in LDL cholesterol between men and women. Males tend to have higher average LDL through early adulthood, but from the 50–54 age bracket onwards, female LDL overtakes male, and the gap widens with each decade.
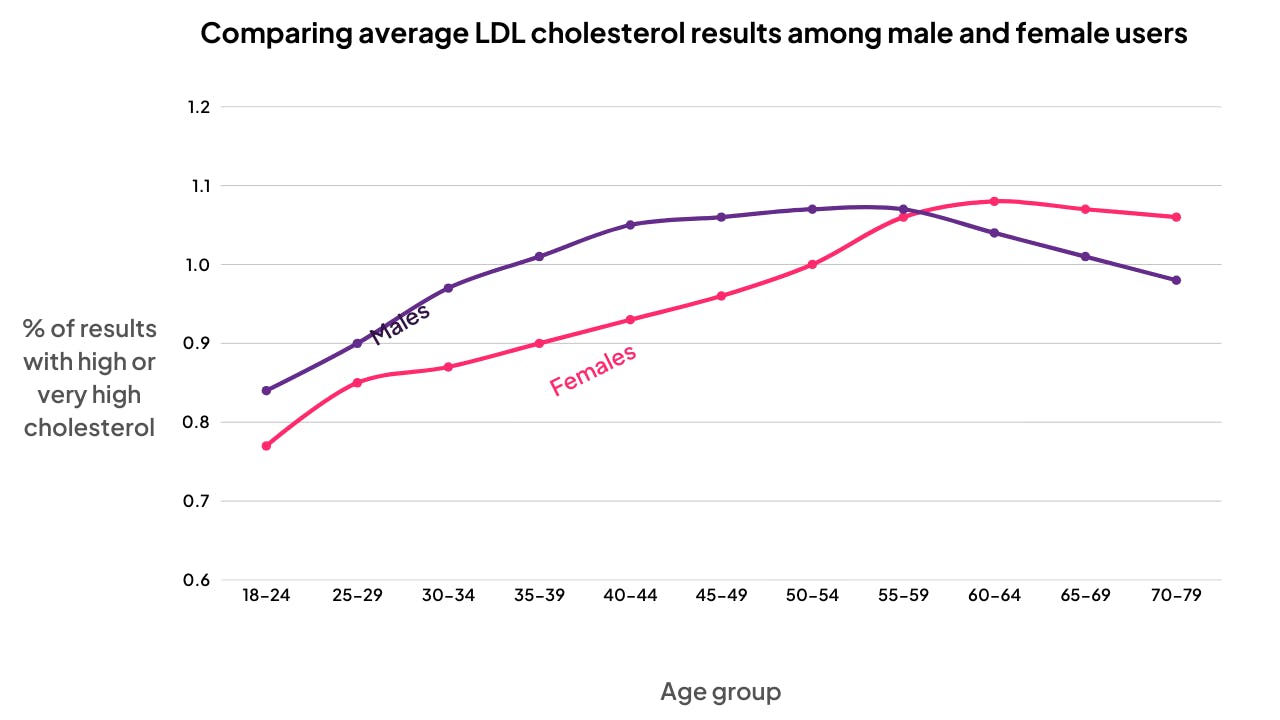
Note: While ApoB is a better predictor of cardiovascular disease, we’ve used LDL for this graph because we have a larger dataset across all age groups.
This maps onto the menopausal transition. Oestrogen helps the liver manage cholesterol levels, so as oestrogen declines at menopause, levels of cholesterol can increase. An analysis from the SWAN study, which followed 1,440 women over a long period of time, confirmed this link.
Understanding this pattern is genuinely useful. It means that for women approaching perimenopause or menopause, keeping an eye on lipids is particularly important. Being equipped with information about how hormonal changes influence health can help you make the changes that support your long-term health.
Takeaway
Cholesterol doesn't respond as quickly or as simply as some other biomarkers. But the data also shows that meaningful differences exist across each of these factors, and that incremental changes in the right direction are associated with measurably better results.
If you're interested in tracking how your lipids respond to changes, ApoB is worth considering alongside LDL cholesterol. Get started by learning more about our home test kits.
Disclaimer: This information is for general educational purposes only and isn’t a substitute for professional medical advice, diagnosis, or treatment. Always speak with a qualified healthcare professional first if you have concerns about your health.
- Anonymised user data, 2025-6
- Khoudary, S. et al. (2023). The independent associations of anti-Müllerian hormone and estradiol levels over the menopause transition with lipids/lipoproteins: The Study of Women's health Across the Nation. https://pubmed.ncbi.nlm.nih.gov/36517413/
- Schoeneck, M. & Iggman, D. (2021). The effects of foods on LDL cholesterol levels: A systematic review of the accumulated evidence from systematic reviews and meta-analyses of randomized controlled trials. https://pubmed.ncbi.nlm.nih.gov/33762150/
- Soffer, D. et al. (2024). Role of apolipoprotein B in the clinical management of cardiovascular risk in adults: An Expert Clinical Consensus from the National Lipid Association. https://www.lipidjournal.com/article/S1933-2874%2824%2900240-X/fulltext
- Suzuki, T. et al. (2025). Lipid Profiles After Changes in Alcohol Consumption Among Adults Undergoing Annual Checkups. https://pubmed.ncbi.nlm.nih.gov/40072433/


