Even if your blood test results show that you’re in the normal range, they still might not fall in the range that’s optimal for your health and longevity — which is where optimal ranges come in. Optimal ranges are evidence-based ranges that are associated with the lowest risk of disease and mortality. These can help overcome a lot of the issues with traditional reference ranges.
What are normal reference ranges?
Reference ranges are used to interpret your blood test results and can tell you whether your levels are normal or abnormal.
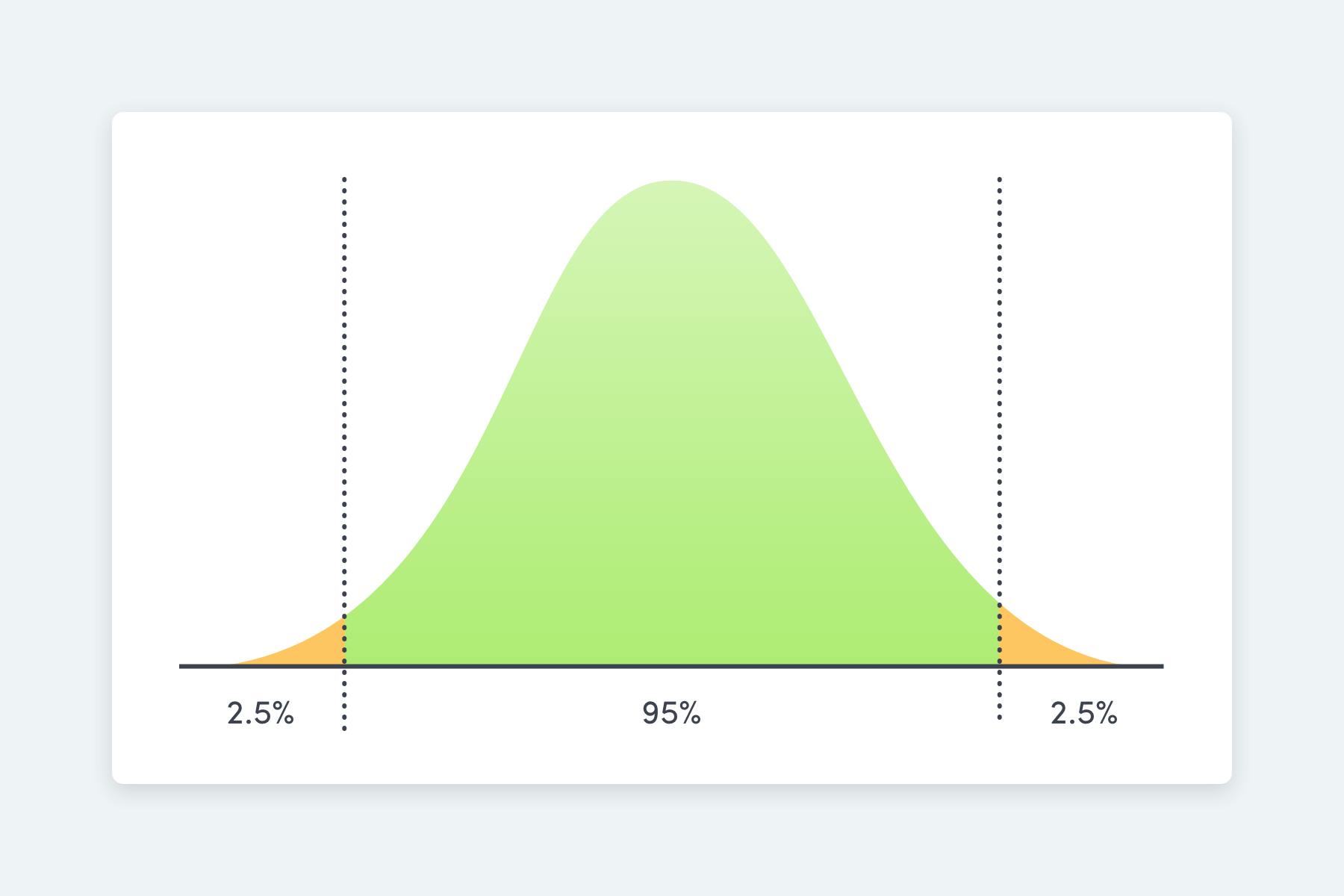
Normal reference ranges are a range of values that are considered normal for a healthy person. These values are usually based on the range that 95% of a healthy population fall into.
A small number of reference ranges are based on whether a value is associated with an increased risk of developing a clinical condition — for example, cholesterol and heart disease.
Issues with normal reference ranges
There are a number of limitations with normal reference ranges, including:
- they’re very black and white and they don’t reflect how complex health is
- they usually don’t take into account how a value links to your risk of developing a disease or your life expectancy
- the studies the ranges are based on often don’t include many people
- some of the population used to determine a range aren’t healthy
A lot of these limitations can be overcome using optimal references ranges.
What are optimal reference ranges?
Using scientific evidence and clinical guidelines, an optimal range is based on whether a range is linked to better health and longevity.
So if your blood test result shows that an analyte, like folate, is within the normal range, it still mightn’t be optimal for your health — meaning you might still be at increased risk for a certain disease or have a lower life expectancy.
A good example of this is vitamin D. Traditional vitamin D guidelines say that if your levels are:
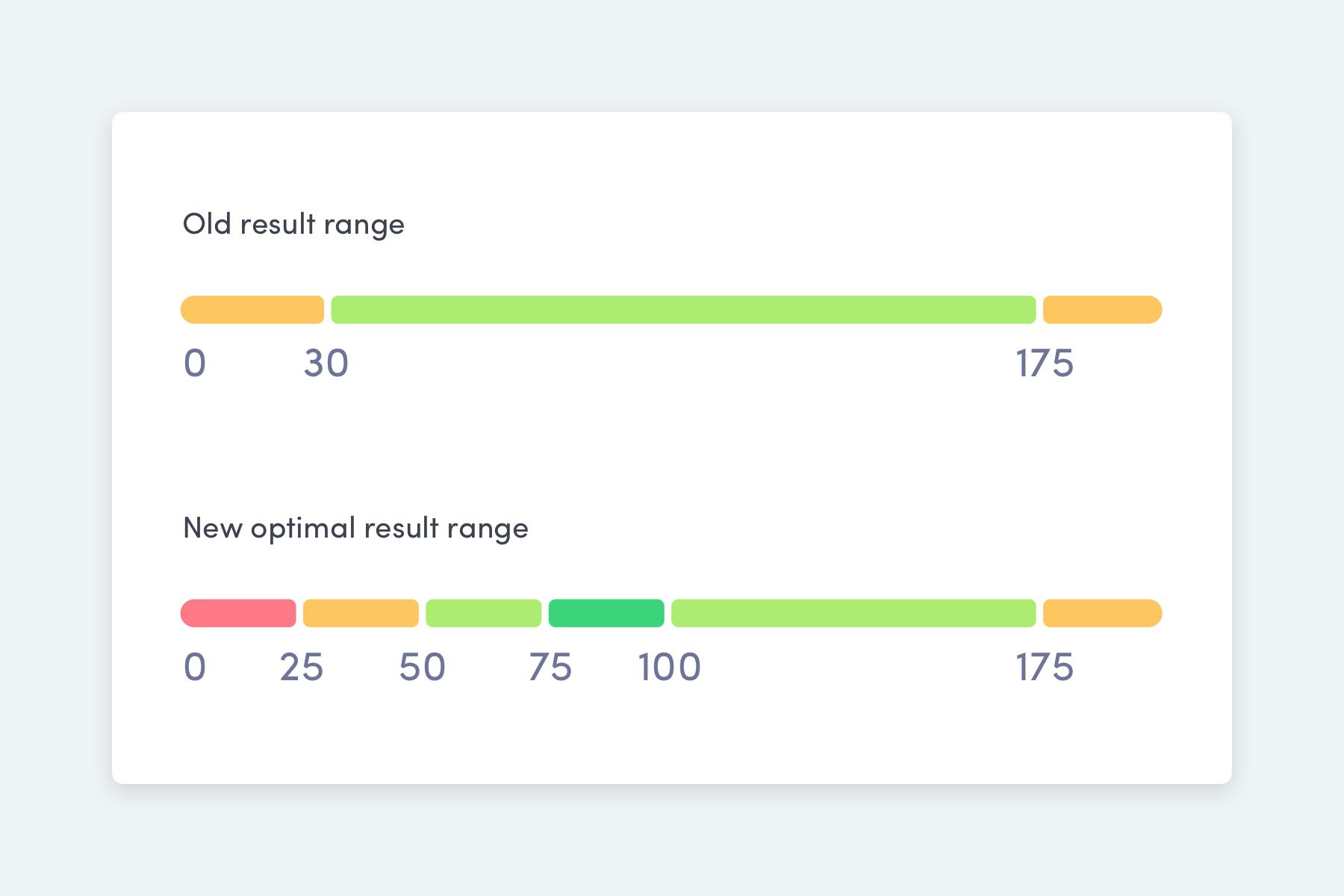
- less than 25 nmol/L you’re deficient
- greater than 50 nmol/L you’re sufficient
This range is only based on the relationship between vitamin D, your bone health, and your risk of osteoporosis.
However, vitamin D is important for many other things, like your muscle and immune health. So the evidence suggests that the optimal range for vitamin D is actually between 75 nmol/L and 100 nmol/L — this is associated with the lowest risk of death (from all causes).
Summary
Normal reference ranges are still very useful and allow healthcare professionals to make informed decisions about your health. But if you really want to optimise your health, optimal ranges can be really useful.
















